Psoriasis
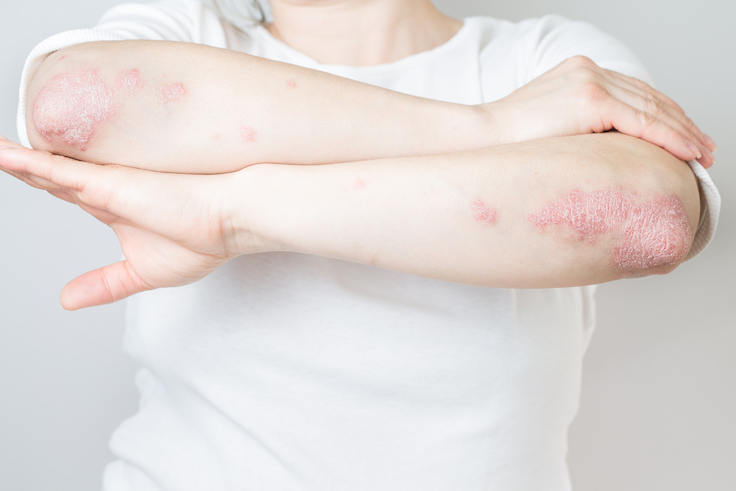
An autoimmune disease that presents itself on the skin can be diagnosed and treated by one of our board-certified dermatologists.
Psoriasis is an autoimmune disease that causes raised, red, scaly patches to appear on the skin. Psoriasis is a chronic disease. Psoriasis is not contagious. Psoriasis can also be associated with arthritis, and less commonly with an increased risk of cardiovascular disease.
There are five types of psoriasis. The type of psoriasis will determine the most appropriate treatment. The types are:
- Plaque psoriasis - the most common form of the disease, it appears as raised, red patches covered with silvery scale, which usually appear on the scalp, knees, elbows and lower back.
- Guttate psoriasis - appears as small, dot-like lesions, often starting in childhood or young adulthood. This type of psoriasis can be triggered by strep infection. Guttate is the second-most common type of psoriasis and affects about 10 percent of psoriasis sufferers.
- Inverse psoriasis - appears as very red lesions in body folds, typically behind the knees, under the arms or in the groin, and it may appear smooth and shiny, It often accompanies another type of psoriasis.
- Pustular psoriasis - appears as white pustules or blisters surrounded by red skin. The pustules contain white blood cells, but it is not an infection, nor is it contagious. It most commonly occurs on the hands or feet.
- Erythrodermic psoriasis - a severe form of psoriasis, it leads to redness over most of the body. It can cause severe itching and pain. This type of psoriasis can cause skin to peel off in sheets and patients can become very sick. It is rare, occurring only in 3 percent of psoriasis sufferers. It generally affects people who have unstable plaque psoriasis.
Causes
Psoriasis is believed to be hereditary with at least 10 percent of the general population inheriting one of more of the genes that create a predisposition to psoriasis. However, only 2-3 percent of the population develop the disease. It is thought that both the predisposition to psoriasis plus exposure to specific external factors, known as “triggers,” causes the disease to appear.
Psoriasis triggers are not universal. What may cause one person’s psoriasis to become active, may not affect another.
Known psoriasis triggers include:
- Stress
- Skin injury
- Certain medications, such as lithium, antimalarials, Inderal, Quinidine, Indomethacin, beta-blockers
- Infection
Because of the hereditary component, people with a family history are at higher risk of developing psoriasis. In the United States, about 7.5 million people have psoriasis. Most people, about 80 percent, have plaque psoriasis.
Psoriasis can begin at any age, but most patients develop it between 15 and 30 years of age or between 50 and 60 years of age.
Treatment
Treating psoriasis can improve a patient’s quality of life by decreasing the appearance of plaques and the associated scaling and itch. There are many different ways to treat psoriasis. The extent of the skin involvement and the presence of arthritis will determine a patient’s appropriate therapy. It is important to keep in mind that individual patients can respond differently to certain therapies.
Treatment options for psoriasis include:
- Biologic Medications - medications that target specific components of the immune system. They are used for moderate to severe psoriasis in patients that have not responded to or cannot take other systemic treatments, or if there is joint involvement. They are given by subcutaneous (just below the surface of the skin) injection or intravenous (IV) infusion. There are risks and side effects associated with the use of biologics which will need to be discussed with your dermatologist.
- Systemic Medications - like biologic medications, systemic medications work by targeting the immune system. They are either oral or injectable prescription drugs that work throughout the body. They are usually used for individuals with moderate to severe psoriasis and psoriatic arthritis. Systemic medications are also used when a patient has failed or cannot use topical medications or UV light therapy.
- Ultraviolet B (UVB) Phototherapy - also referred to as light therapy. This treatment involves consistent exposure of the skin to ultraviolet light under medical supervision. Treatments are done in a doctor’s office or at home with a phototherapy unit.
- Excimer Laser Therapy - was recently approved by the Food and Drug Administration (FDA) for treating chronic, localized plaque psoriasis. It emits a high-intensity beam of ultraviolet light B (UVB). The excimer laser can target select areas of the skin affected by mild to moderate psoriasis, and research indicates it is a particularly effective treatment for scalp psoriasis.
- Pulsed dye laser - is approved for treating chronic, localized plaque psoriasis. Using a dye and different wavelength of light than the excimer laser or other UVB-based treatments, pulsed dye lasers destroy the tiny blood vessels that contribute to the formation of psoriasis lesions.
- Topicals - come in many forms: creams, ointments, shampoo, etc. Topical medications are applied to the affected skin and are usually first-line treatment. They can be used in addition to systemic medications. Topicals can be purchased over the counter or by prescription and include substances such as corticosteriods, saliylic acid, coal tar, zinc pyrithione andcapsaicin.

